What is MIGS?
The goal of all glaucoma surgery is to lower eye pressure. MIGS has become a commonly used abbreviation in the glaucoma world. It stands for minimally invasive glaucoma surgery.
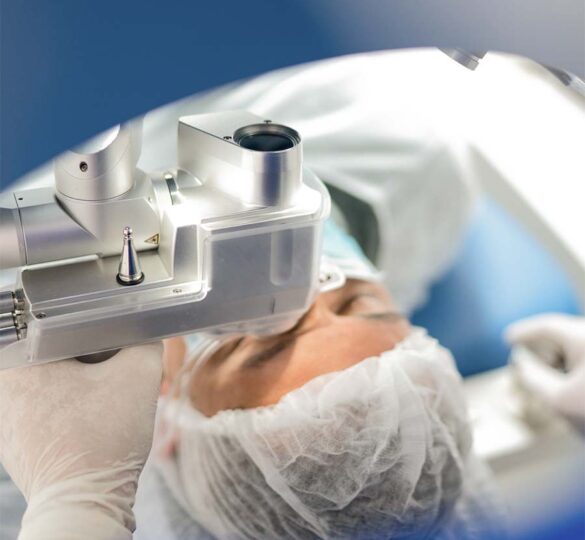
The goal of all glaucoma surgery is to lower eye pressure to prevent or reduce damage to the optic nerve.
Why MIGS?
Standard glaucoma surgeries — trabeculectomy and ExPRESS shunts, external tube-shunts like the Ahmed and Baerveldt styles — are major surgeries. While they are very often effective at lowering eye pressure and preventing progression of glaucoma, they have a long list of potential complications.
The MIGS group of operations have been developed in recent years to reduce some of the complications of most standard glaucoma surgeries.
MIGS procedures work by using microscopic-sized equipment and tiny incisions. While they reduce the incidence of complications, some degree of effectiveness is also traded for the increased safety.
The MIGS group of operations are divided into several categories:
- Miniaturized versions of trabeculectomy
- Trabecular bypass operations
- Totally internal or suprachoroidal shunts
- Milder, gentler versions of laser photocoagulation
Microtrabeculectomies
Using tiny, microscopic-sized tubes that can be inserted into the eye and drain fluid from inside the eye to underneath the outer membrane of the eye (conjunctiva), two new devices seem to make the trabeculectomy operation safer. These devices (the Xen Gel Stent and PRESERFLO [formerly InnFocus] Microshunt) have shown excellent pressure lowering with improved safety over trabeculectomy in studies done outside the United States. (2019 update: These devices have recently been approved for use in the United States).
Trabecular Surgery
Most of the restriction to fluid drainage from the eye rests in the trabecular meshwork. Several operations have been devised using tiny equipment and devices to cut through the trabecular meshwork without damaging any other tissues in the ocular drainage pathway. Using a special contact lens on the eye, a tiny device is inserted into the eye through a tiny incision into the trabecular meshwork under high power microscopic control. The trabecular meshwork can either be destroyed (Trabectome or Trab360) or bypassed using a tiny snorkel-like device (the iStent). These procedures are FDA-approved but generally don’t get the eye pressure very low so are most useful in early to moderate stages of glaucoma.
Suprachoroidal Shunts
Using tiny tubes with very small internal openings, the front of the eye is connected to the suprachoroidal space between the retina and the wall of the eye (Glaukos shunts) to augment the drainage of fluid from the eye. This operation has relatively few serious complications and lowers pressures enough to be useful even in moderately severe glaucoma. (2018 update: See note below regarding the CyPass Micro-Stent).
New Laser Procedures
Previously, laser cyclophotocoagulation was reserved for advanced glaucoma that could not be controlled despite trabeculectomy or tube shunts. The procedures were designed to reduce the fluid-forming capacity of the eye by targeting the delicate tissue (ciliary body) that makes the fluid. They sometimes produced severe inflammation that could reduce vision. Two recent additions to the laser treatment procedures have proven useful even before the glaucoma is far advanced. These are endocyclophotocoagulation and micropulse cyclophotocoagulation.
Summary
Several new approaches to glaucoma surgery show promise for better safety. As with all new procedures, time and much follow-up study are required to see which ones will remain useful for helping glaucoma patients long-term.
Update on CyPass Micro-Stent: On August 29, 2018, Alcon announced an immediate, voluntary market withdrawal of the CyPass Micro-Stent from the global market and advised surgeons to immediately cease further implantation with the CyPass Micro-Stent. Alcon’s decision and corresponding recommendation was based on an analysis of five-year post-surgery data from the COMPASS-XT long-term safety study. At five years, the CyPass Micro-Stent group experienced statistically significant endothelial cell loss compared to the group who underwent cataract surgery alone. For more information: Read the Novartis press release.
Article by Robert L. Stamper, MD. Posted on May 1, 2016; Last reviewed on August 6, 2021.

Robert L. Stamper, MD
Robert L. Stamper, MD is a Distinguished Professor of Clinical Ophthalmology and Director Emeritus of the Glaucoma Service at University of California, San Francisco.