Unique Mapping Device Upgrades Glaucoma Eye Exam to Enhance Individualized Treatment
Optical coherence tomography (OCT) scans offer better diagnostic accuracy by letting doctors see changes inside the eye.
People with glaucoma can only get the most effective treatment when eye doctors can assess what’s happening inside the eye. This sounds obvious, but this task isn’t easy to achieve. Checking eye pressure is one tool, but it’s not 100% dependable because pressure doesn’t always indicate the level of nerve damage accurately.
Optical coherence tomography (OCT) scans offer better diagnostic accuracy by letting doctors see changes inside the eye. It’s encouraging to know that many researchers are devoted to improving OCT technology. Here’s an inside look at the steps bringing glaucoma patients closer to improved and individualized diagnosis and treatment.
How Optical Coherence Tomography Imaging Identifies Glaucoma
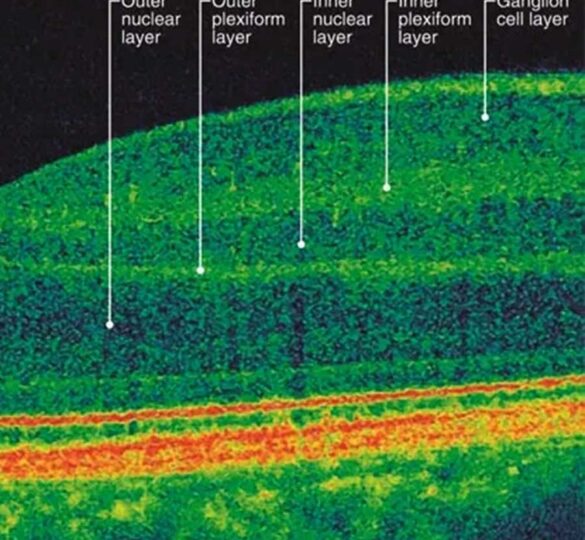
Optical coherence tomography (OCT) uses light rays to take pictures of the retina, using a cross-sectional view that provides doctors with precise measurements of the thickness of the retina and optic nerve tissue that supplies our sight. In the same way that you can only see the different layers of a cake after cutting a slice, OCT reveals the many layers in the wall of the eye, below the visible surface.
The retina consists of multiple layers and each one has a different job, from the photoreceptor cells responsible for catching light to the ganglion cells whose long fibers form the optic nerve to the supporting structures that deliver nutrients. OCT measures the precise thickness of each layer and creates a 3D image. Using these tools, doctors can see changes caused by glaucoma, such as the way nerves thin out when the eye pressure causes damage.
Information from an OCT scan can lead to an earlier diagnosis since optic nerves may appear different in different individuals. Also, thinning of optic nerve may be detected well before damage can be picked up by other tests, such as peripheral vision tests. Then after glaucoma is diagnosed, scans taken over time may show progression of the disease, and whether the treatment is working or needs to be changed.
OCT Advances Lead to Better Glaucoma Diagnosis
OCT has been around for decades but scientists continue working to improve the technology. One important advance came in the form of OCT devices with higher resolution, revealing even more about the eye than was visible before. For example, thanks to OCT devices with increased resolution, the optic disc was able to be captured by the scan. The optic disc is the area where the optic nerve leaves the eye on its way to the brain. Doctors now use OCT to visualize the rim around the optic disc, looking for changes in its width. Rim width is a key indicator of glaucoma deterioration.
This was a first step, but experts knew that optic disc measurements aren’t always precise. They realized they needed to find stable landmarks that could be used to accurately measure optic rim changes. After years spent examining hundreds of OCT scans, two microscopic landmarks emerged: the fovea and Bruch’s membrane.
The fovea is a small dimple in the middle of the retina that’s responsible for sharp vision and color perception. It is far from the optic disc and is unaffected usually until late in the disease. Bruch’s membrane, a layer of tissue behind the retina, stops at the optic nerve, so the center of the Bruch’s membrane opening also marks the center of the optic disc. When a line is drawn between the two landmarks and compared to other measurements inside the eye, changes in the size of the optic rim can be precisely determined. This piece of information ushered in a new era of research as experts explore novel ways to use these fixed landmarks in the field of glaucoma and other eye diseases.
New Upgrades Individualize Glaucoma Eye Exams
In the meantime, an exciting advance came from Heidelberg Engineering, a company that manufactures an imaging device called the Spectralis OCT. Experts at the company developed a software upgrade called the Glaucoma Module Premium Edition, which was approved by the FDA in September 2016. When it’s uploaded to the Spectralis OCT, this innovative add-on uses the two landmarks to create an anatomic map that’s unique to each person. Individualized maps from each new OTC scan can be compared, which means doctors can customize treatments and monitor glaucoma progression.
First posted February 16, 2017; Last reviewed June 22, 2022