Glaucoma Surgery: What To Expect
Several surgical treatments are available, depending on the type and stage of glaucoma.
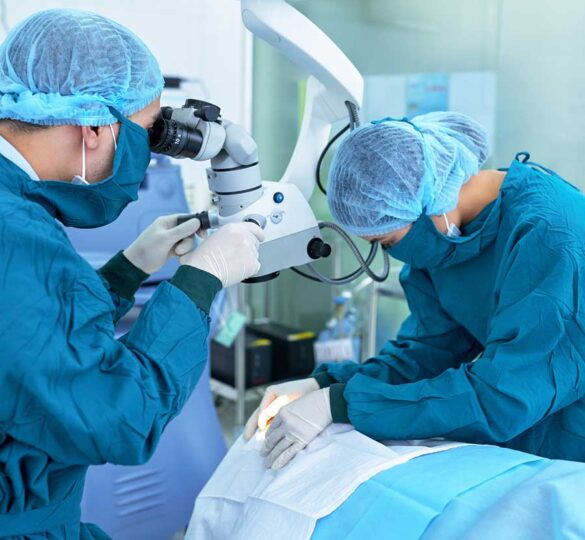
Glaucoma, often dubbed the “silent thief of sight,” is a formidable ocular disease characterized by progressive optic nerve damage, primarily due to elevated intraocular pressure (IOP), leading to progressive vision loss. When medical therapies like eye drops or laser treatments fail to manage the pressure adequately, glaucoma surgery emerges as a vital intervention.
The primary goal of glaucoma surgery is to reduce the IOP by improving the eye’s natural drainage system or creating new drainage pathways. With advancements in medical technology, glaucoma surgeries have evolved significantly, offering patients better outcomes, reduced complications, and improved postoperative recovery. Continue reading for information on types of surgeries, insights into what to expect when having glaucoma surgery, and recovery tips.
Types of Glaucoma Surgery
Several surgical treatments are available, depending on the type and stage of glaucoma. Depending on several factors, your doctor will determine the type of surgery you need. Most glaucoma surgeries are outpatient procedures, lasting approximately 20 to 40 minutes, usually done in a day surgery unit of a hospital or an ambulatory surgery center.
After the procedure, patients are typically monitored for a short time to ensure there are no immediate complications, then discharged with post-operative instructions and medications. Scheduled follow-up appointments monitor the eye’s healing process and ensure the surgery effectively controls IOP.
Of course, the details can vary based on the type of glaucoma surgery performed, the patient’s overall health, potential complications, and the surgeon’s preference.
Some of the most common ones include:
- Trabeculectomy
A surgical instrument creates a small opening in the sclera, or sidewall of the eye, creating a new pathway for fluid flow.
- Minimally Invasive Glaucoma Surgery (MIGS)
As the name suggests, MIGS is a group of surgical procedures designed to be minimally invasive, often using microscopic-sized equipment and tiny incisions. These methods offer an intermediate solution between medical treatment (eye drops) and more invasive surgical treatments.
- Tube Shunt Surgery
Typically reserved for patients whose glaucoma hasn’t responded to other treatments like eye drops, laser therapy, or traditional trabeculectomy surgery, the main goal of this surgery is to reduce the IOP by inserting a tube and reservoir device into the eye to drain aqueous humor.
Before Surgery
- You’ll have a pre-operative appointment to review your medical history, take eye measurements, and discuss the surgical procedure with your ophthalmologist.
- You may be prescribed antibiotic eye drops to use for several days before surgery to prevent infection.
- Your doctor may recommend stopping certain medications like blood thinners, aspirin, anti-inflammatories, or supplements before surgery.
Recovery After Glaucoma Surgery
Post-operative care following glaucoma surgery is not only essential but indispensable. The process of healing is equally important to the surgery’s success. Without rigorous post-operative diligence, patients face a heightened threat of infections and other complications that might negate the surgical benefits and even create further vision deterioration. Following your doctor’s instructions is pivotal to optimal results.
- Follow the Medication Schedule: Ensure you take all prescribed medications, including eye drops, to prevent infection and control inflammation.
- Avoid Strenuous Activity: Heavy lifting, bending, or strenuous activity can increase eye pressure. Consult your doctor about when you can resume normal activities.
- Protect Your Eyes: Wear sunglasses to shield your eyes from the sun and avoid any potential irritants like dust.
- Have Regular Check-ups: Attend all post-operative appointments to allow your doctor to monitor healing and ensure no complications arise.
- Watch for Signs of Complications: Redness, severe pain, or decreased vision might indicate a problem. If you experience any unusual symptoms, contact your doctor immediately.
Glaucoma surgery is a crucial intervention that can prevent further vision loss. Being informed about the procedure and following recovery guidelines can aid in a smoother healing process. Always consult with your ophthalmologist about the best treatment options for your condition.
Help Us Provide Hope
Glaucoma can be successfully treated with early diagnosis, treatment, and careful monitoring, preventing it from causing permanent and significant vision impairment.
The diligent work of researchers continues to lead to a better understanding of glaucoma every day. As a result, there’s great hope for new and improved treatments, including superior drug delivery methods, laser treatments, and less invasive surgical techniques. You can help make that happen!
Your support can help dedicated researchers continue to discover the causes and cures for glaucoma. In addition, your donations give hope to those living with glaucoma and accelerate our search for a cure.
Posted on December 4, 2023. Reviewed for medical accuracy by Sandra F. Sieminski, MD.

Sandra F. Sieminski, MD
Sandra Sieminski, MD is a glaucoma and cataract specialist at the Ross Eye Institute and is the Director of Glaucoma Services. She also serves as the Clinical Vice Chair of the Department of Ophthalmology for the Jacobs School of Medicine and Biomedical Sciences, University at Buffalo/State University of New York (SUNY).